How to Check Medication Strength and Quantity on Prescription Labels
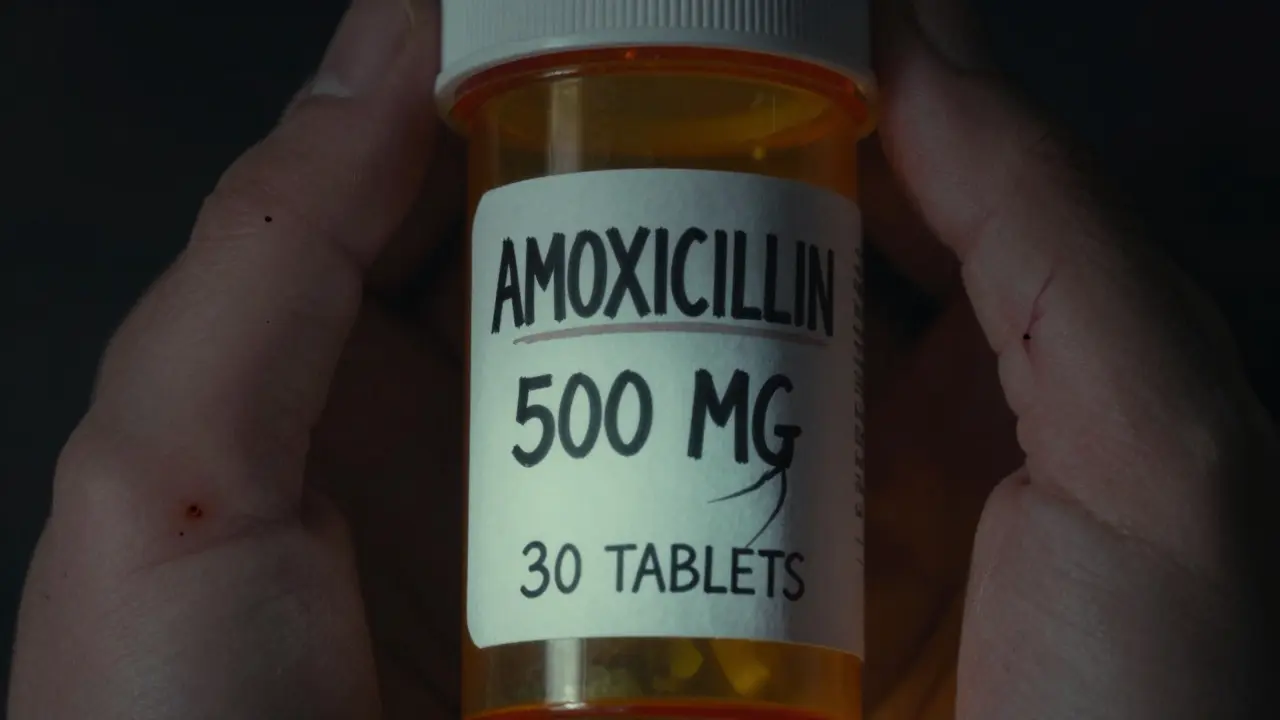
Every time you pick up a prescription, you’re holding a safety check that could prevent a life-threatening mistake. But if you don’t know what to look for, that label might as well be written in another language. The truth is, medication strength and quantity on prescription labels aren’t just fine print-they’re your last line of defense against dangerous errors. And you don’t need a medical degree to read them. Just a little attention, a few simple steps, and the right questions to ask.
What Strength and Quantity Actually Mean
Strength tells you how much active drug is in each dose. Quantity tells you how much total medicine you got. Sounds simple? It should be. But confusion here is one of the top causes of medication errors.
For example, if your label says AMOXICILLIN 500 MG, that means each tablet or capsule contains 500 milligrams of the antibiotic. If you’re supposed to take one tablet twice a day, and you grab two by mistake thinking they’re weaker, you’ve just doubled your dose. That’s not just a mistake-it’s a risk.
Liquid medications are trickier. You might see something like 250 MG/5 ML. That means every 5 milliliters (about one teaspoon) contains 250 milligrams. If you misread it as 250 MG per milliliter, you’re giving yourself five times the intended dose. That’s how pediatric overdoses happen.
Topical creams? They often show strength as a percentage. HYDROCORTISONE 1% CREAM means 1 gram of the drug is in every 100 grams of cream. If you think it’s 10%, you might use way too much.
Units matter. mg (milligrams), mcg (micrograms), and IU (international units) are not interchangeable. A microgram is 1,000 times smaller than a milligram. Confusing them can be deadly. That’s why FDA rules now require full words like “microgram” instead of “mcg” on some labels-but not all pharmacies follow that yet.
Where to Find Strength and Quantity on the Label
Look right after the drug name. Most pharmacies put the strength directly beneath or in parentheses after the medication. CVS puts it below the name. Walgreens often writes it like this: AMOXICILLIN (500 MG). Independent pharmacies might handwrite it-so double-check the handwriting.
Quantity is usually near the bottom. It’ll say something like:
- 30 TABLETS
- 120 ML
- 30 GRAMS
This is the total amount in the bottle. It doesn’t tell you how much to take each time. That’s on your prescription or the instructions. But if you get 60 tablets instead of 30, you might think you’re getting a refill when you’re not. Or worse-you might think you’re out when you still have half left.
Some labels include extra info: “Take 1 tablet daily” or “Use as directed.” Don’t rely on those alone. Always cross-check the strength and quantity against what your doctor wrote.
How to Verify Your Label Against Your Prescription
You have a right to ask for your original prescription copy. Most pharmacies keep it on file. Compare the label to what your doctor wrote. If your doctor prescribed AMOXICILLIN 500 MG and you got 250 MG, that’s an error. Even if the pill looks the same, strength can vary.
Here’s a quick 4-step check:
- Find the drug name-make sure it matches what your doctor prescribed.
- Locate the strength-check the number and unit (mg, mcg, etc.).
- Check the quantity-does it match how many pills or how much liquid you were told to expect?
- Match the Rx number-the number on the label should match the one on your prescription receipt.
Don’t assume the pharmacist got it right. In 2022, the American Society of Health-System Pharmacists reported that over 1.3 million medication errors happened in the U.S. that year. About 22% of them were due to misreading strength or quantity on labels.

Common Mistakes People Make (And How to Avoid Them)
Here are the mistakes you’re most likely to make-and how to stop them:
- Misreading decimals - “0.25 mg” looks like “25 mg” if you squint. Always pause and ask: Is there a decimal point? Use a magnifying app on your phone if needed.
- Confusing total quantity with daily dose - You got 30 tablets. Does that mean you take 30 a day? No. It means you have 30 total. Check the instructions for daily amount.
- Assuming brand names = strength - A brand like “Lipitor” doesn’t tell you the dose. You need to see “ATORVASTATIN 20 MG.” Generic names are more reliable.
- Ignoring liquid ratios - “5 MG/5 ML” isn’t the same as “5 MG.” You need to measure the volume. A syringe or dosing cup is required. Never use a kitchen spoon.
- Not checking high-risk meds - Blood thinners, insulin, seizure drugs, and heart medications have narrow safety margins. Always double-check these. The FDA says these account for 68% of fatal dosing errors.
One patient in Wisconsin caught an error after her blood pressure pill changed from 2.5 mg to 10 mg. The pill looked different, but she didn’t know why-until she checked the label. She called the pharmacy. They had filled the wrong strength. She saved herself from a dangerous spike in blood pressure.
Tools That Help You Verify Labels
You don’t have to do this alone. Pharmacies are required to offer help:
- QR codes - Many labels now have QR codes. Scan them with your phone. They’ll link to the FDA’s official medication guide, showing exact dosing, warnings, and strength details.
- High-contrast labels - If you have trouble reading small print, ask for a large-print or bold-font label. Over 89% of chain pharmacies offer this for free.
- Mobile apps - Apps like MyTherapy or Medisafe let you scan your prescription barcode and compare the label to your recorded meds. Some even alert you if the strength doesn’t match.
- Pharmacist consultation - Ask the pharmacist to walk you through it. No charge. No judgment. They’re trained to help you understand.
In 2023, a JAMA Internal Medicine study found that pharmacies using barcode scanning reduced verification time from 47 seconds to just 8 seconds-and cut errors by 34%. But even with tech, your eyes still matter.

What to Do If Something Looks Wrong
If the strength or quantity doesn’t match what you expect:
- Don’t take it.
- Call the pharmacy. Ask: “Can you confirm the strength on this label matches my prescription?”
- If they say it’s correct, ask to speak to the pharmacist on duty. Ask them to show you the original prescription.
- If you’re still unsure, take the label to another pharmacy. They can check it against the prescriber’s record.
- Report it. The FDA’s MedWatch system lets you report errors anonymously. This helps improve safety for everyone.
One Reddit user, u/MedSafetyMom, caught her son’s amoxicillin dose doubled because the pharmacy gave 500 mg/5 mL instead of 250 mg/5 mL. She noticed because she’d checked the last refill. She called, the pharmacy apologized, and they re-filled it. She says: “I didn’t know I could do that. Now I do.”
Why This Matters More Than Ever
People are taking more medications than ever. The average Medicare beneficiary takes 4.7 prescriptions. That’s a lot of labels to read. And with aging populations and more complex drugs, the risk of confusion is rising.
Studies show that patients who check their labels prevent 28% of potential dosing errors. That’s not just a number-it’s lives. Especially for older adults, people with low health literacy, or those managing multiple conditions.
By 2026, new standards will require red borders around strength info for high-risk drugs. Color-coding will help. But until then, your eyes and questions are the best tools you have.
What if the strength on my label says mcg instead of mg?
That’s a major red flag. A microgram (mcg) is 1,000 times smaller than a milligram (mg). If your prescription says 5 mg but the label says 5 mcg, you’re being given a dose 1,000 times too low-or worse, if it’s reversed, 1,000 times too high. Call the pharmacy immediately. Never take it without confirming.
Can I trust the pill imprint to match the strength?
Pill imprints (letters/numbers on tablets) help identify the drug, but not always the strength. Two different strengths of the same drug can look identical. For example, a 10 mg and a 20 mg pill of the same medicine might have the same imprint. Always check the label-not the pill.
Why do some labels have brand names and others have generic names?
It depends on your prescription and pharmacy policy. Some doctors write the brand name; others write the generic. Pharmacies can substitute generic versions unless the doctor says “dispense as written.” Always look for the generic name first-it’s the active ingredient. Brand names are just marketing names. The strength is what matters.
Do I need to check my label every time I refill?
Yes. Medication errors happen during refills more often than first fills. A pharmacy might switch suppliers, change manufacturers, or accidentally pull the wrong bottle. Even if it’s the same drug, strength can change. Make checking the label part of your routine-like checking the expiration date.
What should I do if I notice a pattern of errors at my pharmacy?
Switch pharmacies. Your health isn’t worth the risk. You can also report the issue to your state pharmacy board or the FDA’s MedWatch system. Thousands of people do this every year. It helps improve safety standards. You’re not just protecting yourself-you’re helping others.
Final Thought: Your Eyes Are Your Best Safety Tool
Technology helps. Apps, QR codes, and barcode scanners are great. But none of them replace your own attention. You’re the one who takes the pill. You’re the one who knows your body. If something feels off, it probably is. Take a second. Read the label. Ask the question. Don’t be afraid to say, “I’m not sure about this.” That one moment of doubt could save your life-or someone else’s.




Srividhya Srinivasan
Oh, PLEASE tell me you’re not one of those people who just ‘trusts the pharmacy’… I mean, really? You think they’re not cutting corners? I’ve seen pharmacists hand me a bottle labeled ‘10 MG’ when the script said ‘10 mcg’-and they laughed. Laughed! I had to threaten to call the state board just to get them to recheck. And don’t get me started on the ‘generic’ that turned out to be a different salt entirely. You think you’re safe? You’re one typo away from a coma. Always. Check. The. Label. Always.
Prathamesh Ghodke
Love this breakdown. Seriously. I’m a pharmacist in Mumbai, and I can’t tell you how many times I’ve had to sit with someone for 15 minutes explaining that ‘500 mg’ isn’t ‘500 mcg’-and no, your ‘tiny pill’ isn’t ‘weaker’ just because it’s smaller. We’re not trying to trick you. But yeah, labels are messy. My advice? Take a photo of the label and compare it to your doctor’s note. If it’s a mismatch, come back. No judgment. We’ve all been there. And hey-thanks for reminding people to ask. That’s half the battle.
Justin Archuletta
YES. YES. YES.
Check the label.
Don’t assume.
Ask.
Take a picture.
Double-check.
Repeat.
You’re not paranoid-you’re prepared.
And if someone says you’re overreacting? Tell them to Google ‘insulin dosing error’.
Sanjana Rajan
Ugh. Another ‘read the label’ lecture. Like that’s going to stop Big Pharma from slipping in 10x stronger generics. You think pharmacies are innocent? Please. They’re profit machines. They don’t care if you live or die as long as the script clears. And don’t even get me started on QR codes-those are just tracking devices. Scanning them means they now know what meds you’re taking, when, and where. This whole thing is a distraction. Real change? Ban generics. Ban all of it. Only brand-name. No exceptions.
Kyle Young
It’s fascinating how the human body has evolved to rely on external systems-pharmacies, labels, prescriptions-to regulate its internal chemistry. And yet, we’re told to trust these systems implicitly. But when we do, we surrender agency. The label becomes a proxy for authority. What if authority is fallible? What if the system, designed to protect, is instead a conduit for cascading error? The real question isn’t ‘How do I read the label?’-it’s ‘Why do I have to?’
Aileen Nasywa Shabira
Oh wow, another ‘be vigilant’ PSA. How quaint. You know what’s *really* dangerous? The fact that your doctor didn’t even write the prescription correctly in the first place. Or that your insurance forced a switch to a generic you’ve never taken. Or that your pharmacy uses a bot to fill scripts and the AI misreads handwriting. You’re not ‘saving lives’ by checking labels-you’re patching a broken system with duct tape. And frankly? It’s exhausting.
Kendrick Heyward
My aunt died because of this. She took a pill that said ‘2.5 mg’ but it was actually ‘25 mg’-and they didn’t even apologize. Just said ‘mistake’. I cried for weeks. Now I take a photo of every label. I text it to my sister. I call the pharmacy twice. I’m not ‘overly cautious’-I’m surviving. If you’re not doing this? You’re playing Russian roulette with your life. 💔
lawanna major
The structure of pharmaceutical labeling is a fascinating intersection of regulatory compliance, human cognition, and systemic fragility. The fact that we rely on visual parsing of alphanumeric codes-often under poor lighting, with aging eyes, and without standardized typography-creates a perfect storm for error. The FDA’s push toward full-word units (‘microgram’ over ‘mcg’) is a step toward cognitive accessibility, but implementation remains patchy. We must not only educate patients but redesign the interface: larger fonts, color-coded risk tiers, mandatory audio verification at pickup. The burden shouldn’t fall on the patient. It should be engineered out of the system.
Ryan Voeltner
Thank you for this comprehensive overview. The clarity with which you present the risks and solutions is both necessary and commendable. In a world where healthcare complexity continues to rise, such foundational knowledge empowers individuals to participate meaningfully in their own care. It is a small but vital act of self-advocacy that carries profound implications. I hope this message reaches those who need it most.
Linda Olsson
Oh, so now we’re supposed to become amateur pharmacists? How convenient. While you’re out here checking labels, the real issue is that pharmacies are outsourcing fill lines to countries with zero oversight. Did you know most pills in the U.S. are manufactured in India or China? And the ‘label’? Printed by a third-party vendor who doesn’t even speak English. You think your ‘500 mg’ is 500 mg? It’s probably 487. And they’ll never admit it. This isn’t safety-it’s performance art.
Ayan Khan
This is beautiful. I’ve seen elderly parents in Delhi misread labels because the text was too small, and their children were far away. We need community health volunteers-people who can sit with elders, read the label aloud, explain the difference between mg and mcg. Technology helps, but human presence? That’s the real safety net. Let’s train more of them. Let’s make this part of our social fabric. Not just a warning- a ritual of care.
Emily Hager
How dare you suggest that patients should be responsible for verifying their own medication? This is a systemic failure of the medical-industrial complex. The burden of vigilance should not fall on the vulnerable. The pharmacy should be held accountable. The pharmacist should be legally liable. The manufacturer should be fined. You’re normalizing negligence by asking people to ‘check the label.’ That’s not empowerment-that’s victim-blaming.
Melissa Starks
I used to be one of those people who just took whatever the pharmacist handed me. Then my mom had a stroke because they gave her a blood thinner that was 5x stronger than prescribed. She’s fine now, but I’ll never forget the look on her face when she realized what happened. So now? I’m the label-checking queen. I take pics. I write notes. I call the pharmacy at 10 p.m. if I’m unsure. I even made a spreadsheet. My kids think I’m crazy. But I’m alive. And so is she. If you’re not doing this? You’re not just being lazy-you’re putting your life in someone else’s hands. And that’s not okay. Please. Just check. Once. For your future self.
Lauren Volpi
Ugh. Another ‘check your label’ lecture from the U.S. of A. Meanwhile, in real countries, people get their meds from the corner shop and trust the guy who’s been doing it for 30 years. You’re so obsessed with bureaucracy and QR codes you’ve forgotten what trust looks like. Maybe the problem isn’t the label-it’s your paranoia. Chill. The world isn’t out to kill you. Probably.
Kal Lambert
Simple. Smart. Necessary.
Check the label.
Ask the pharmacist.
Trust but verify.
It takes 30 seconds.
It could save your life.